CLinical Volume
The combination of bountiful volume in every facet of cardiovascular and thoracic surgery at Loyola, Christ, and the Hines VA Hospital imparts confidence and skill to our residents. This page will describe the variety of cases available at each site, but the bottom line is the experience reported by our most recent graduates to the ACGME in their final case logs, downloadable here:
| 2019_resident_a_acgme_final_case_log.pdf | |
| File Size: | 253 kb |
| File Type: | |
| 2019_resident_b_acgme_final_case_log.pdf | |
| File Size: | 254 kb |
| File Type: | |
| 2020_resident_a_acgme_final_case_log.pdf | |
| File Size: | 288 kb |
| File Type: | |
| 2020_resident_b_acgme_final_case_log.pdf | |
| File Size: | 288 kb |
| File Type: | |
| 2021_resident_a_acgme_final_case_log.pdf | |
| File Size: | 255 kb |
| File Type: | |
| 2021_resident_b_acgme_final_case_log.pdf | |
| File Size: | 254 kb |
| File Type: | |
| 2022_resident_a_acgme_final_case_log.pdf | |
| File Size: | 212 kb |
| File Type: | |
| 2022_resident_b_acgme_final_case_log.pdf | |
| File Size: | 212 kb |
| File Type: | |
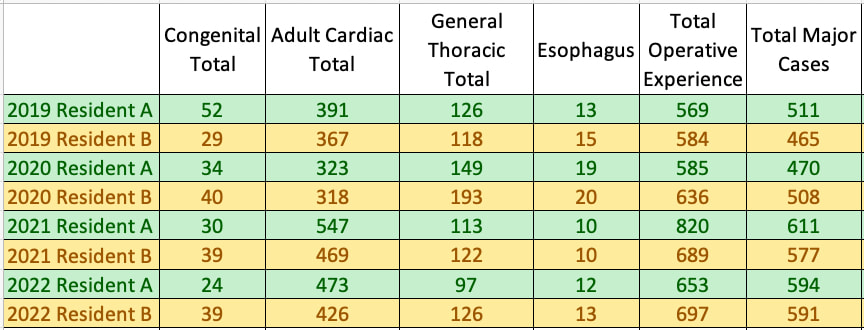
This table summarizes the information that can be gleaned from a detailed examination of the case logs listed above.
Please note that this period covers the entirety of the COVID-19 pandemic, and that the impact of the pandemic on clinical workflow and bed occupancy did not have an appreciable impact on resident training volume.
Loyola Thoracic And ADULT CARDIOVASCULAR Surgery
With a very active heart and lung transplant program, as well as its regional leadership in advanced technology such as endovascular grafting, percutaneous valve implantation, and destination therapy circulatory support, Loyola performs cardiovascular and thoracic procedures far in excess of what can be staffed by our complement of categorical residents. This provides an environment where residents can involve themselves with those cases they believe will most benefit their education, while our surgical assistants cover the remainder. Similarly, our dedicated Cardiovascular and Thoracic Intensive Care Unit is staffed by Anesthesia residents who carry out the majority of the 'front-line' care with the oversight of our trainees, so that our Thoracic residents are freed to pursue their technical development while building their clinical management skills. On the wards and in clinic, our team of Nurse Clinicians and Physician Assistants effectively manage inpatient and outpatient care with resident involvement as necessary.
Loyola is a regional leader in thoracoabdominal aortic surgery, lung and heart transplantation, as well as mechanical circulatory support. A substantial amount of our volume is valvular. Since the time of the early Heartport experience, Loyola has been a leader in minimally invasive valvular surgery, with particular preeminence in advanced mitral repair, and valve sparing aortic root procedures. Our transcatheter aortic valve implantation experience includes both Medtronic CoreValve and Edward Sapien devices.
Loyola is a regional leader in thoracoabdominal aortic surgery, lung and heart transplantation, as well as mechanical circulatory support. A substantial amount of our volume is valvular. Since the time of the early Heartport experience, Loyola has been a leader in minimally invasive valvular surgery, with particular preeminence in advanced mitral repair, and valve sparing aortic root procedures. Our transcatheter aortic valve implantation experience includes both Medtronic CoreValve and Edward Sapien devices.
Loyola Thoracic Surgery
Loyola Thoracic Surgery has always drawn complex patients from around the Midwest, as has the Cardinal Bernardin Cancer Center, which offers our patients close coordination of our care with multi-disciplinary oncology teams. The Thoracic Section also features a very busy lung transplant service, as well as experience with robot assisted surgery. In the first quarter of 2016, Dr. Wickii Vigneswaran joined the faculty as the Chief of the Thoracic Section after several years on the faculty of the University of Chicago. He brings cutting edge minimally invasive skills and a particular interest in mesothelioma, robotic and esophageal procedures to supplement the traditional strength of the resident's experience. Dr. Lubawski and he have grown the Thoracic volume in 2016 by over 55% from the previous year. Academic year 2017 finished with 354 major thoracic cases. This number does not include 43 lung transplants performed during that academic year. In August of 2020, Dr. Zaid Abdelsattar and Dr. Wissam Raad joined the Section. Dr. Abdelsattar applies robotic surgery skills learned at the Mayo Clinic to the full spectrum of thoracic disease at Loyola and the Hines VA Hospital. Dr. Raad is very experienced in robot assisted thoracic surgery, and divides his time between Loyola and St. Joseph's Hospital in Joliet.
Hines VA Hospital Cardiothoracic Surgery
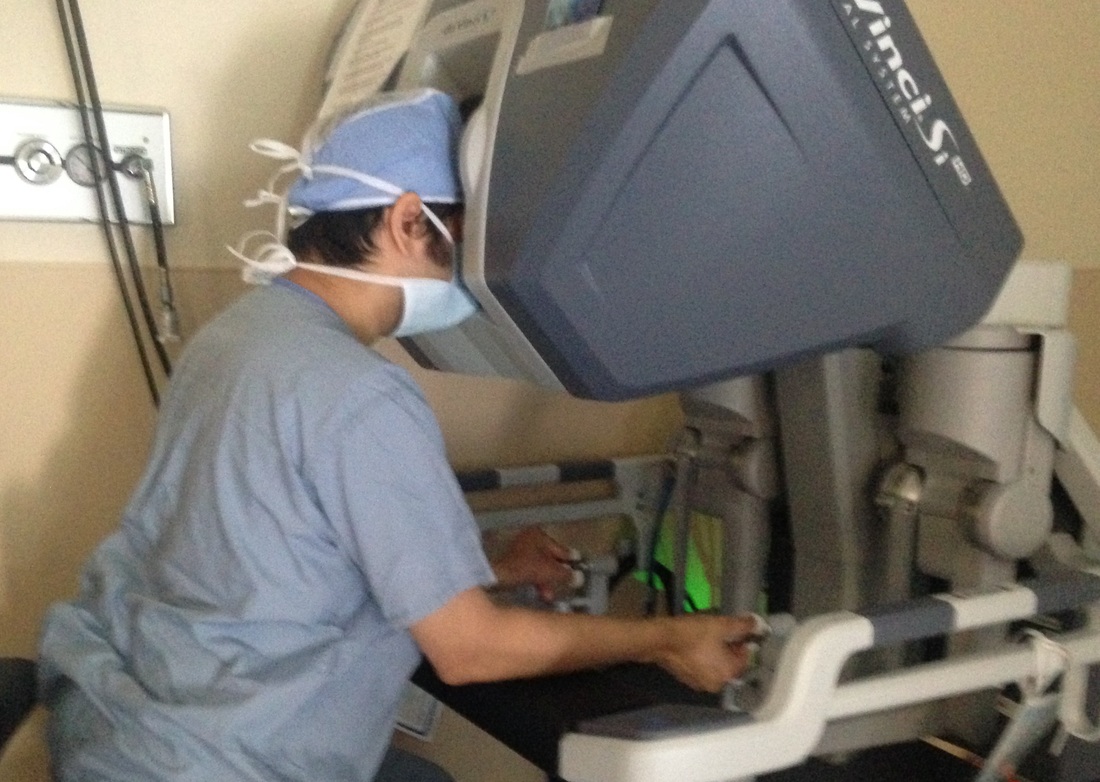
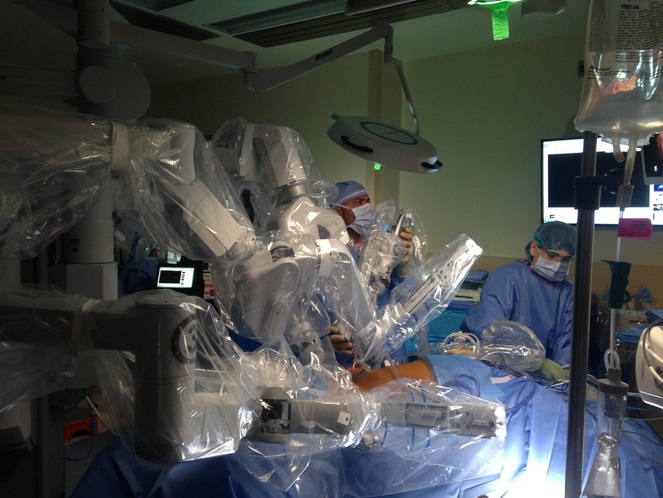 Robotic Lung Procedure at the Hines VA Hospital
Robotic Lung Procedure at the Hines VA Hospital
The Hines VA Hospital, physically contiguous with Loyola University Medical Center, is an invaluable training site for the residency program, and a favorite rotation for our residents, both for the opportunity to care for our nation's veterans, and for the chance to "put together" what they have learned about technique, clinical decision making, and practice management in an environment where they are allowed carefully supervised autonomy. The recently renovated operating rooms, intensive care units, and wards handle complex cases, including minimally invasive procedures, referred from throughout VISN 12. The Hines VA service screens about 450 patients per quarter. Hines VA has three DaVinci Robotic operating rooms, two Xi and one Si platforms.
Congenital Cardiothoracic Surgery
Though some congenital cardiothoracic cases are performed at Loyola, the vast majority of the resident experience in this field is acquired at Christ Hospital, where Dr. Vricella's team tackles the full spectrum of complex repairs of congenital malformations. Residents are typically extremely satisfied with the technical education they receive from our faculty there, As American Board of Thoracic Surgery case requirements are easily satisfied in a one month rotation, at the request of our residents, and in alignment with other traditional track programs, this rotation block has been changed to one month duration, with the other two months of the block assigned to Thoracic Surgery at Loyola.